
Fifteen years ago, when Faith Mudangwe was 14, she became a caregiver to her dying mother. She looked on helplessly, limited by scarce resources and poor access to health facilities, as her mother’s weight plummeted, and then as she began to bleed non-stop.
“After my mother’s death, life became very hard for us as a family because we had no one to look after us.”
– Faith Mudangwe, who lost her mother to cervical cancer
After months of visiting various hospitals, Mudangwe’s mother was put on home-based hospice care. She died aged 35, leaving her young family effectively orphaned. Faith’s father married another woman and started a new family. Faith, the eldest child, felt the responsibility for her family come to rest on her shoulders.
“After my mother’s death, life became very hard for us as a family because we had no one to look after us and provide for the family,” Mudangwe, now 29, recalls. “Everything happened so fast, we didn’t know what to do, or where to turn to.”
The hospital confirmed cervical cancer and HIV as the joint cause of death. Both conditions were unfortunately diagnosed very late, after years of shuffling between faith healers, in desperate search for spiritual intervention, but all to no avail, on a continent where cervical cancer screening is estimated at just 12%.
It’s unfortunately not an uncommon story. Close to 2000 Zimbabwean women die slow painful deaths from the disease annually.
That’s all the more alarming because cervical cancer is vaccine-preventable. More than 95% of cervical cancer cases are caused by infection with the human papillomavirus (HPV) according to WHO. Zimbabwe’s nationwide rollout of the HPV vaccine began in 2018. According to country administrative data , coverage stood at an estimated 80% in 2019. Still, 62 women out of every 100,000 are diagnosed with the illness each year.
COVID-19’s disruptions promised a potential setback. Aiming to tackle more than one trouble spot at a time, the country recently undertook an integrated vaccination campaign, bundling HPV, tetanus and COVID-19 immunisation. The HPV vaccination targeted around 800,000 young girls aged ten to 14 years.
“These days, young girls are getting sexually active as early as 12 years, and by giving them the HPV vaccine early, it will help prevent them from cervical cancer,”said Judith Gwati, a health worker.
Other vaccination programmes have been disturbed by the COVID-19 pandemic, while resources and efforts were channelled to combat the novel coronavirus, which has killed more than 5,700 people since January 2020.

Credit: Albrecht Fietz from Pixabay
“The issue of administering HPV vaccines, as much as it is an important cancer prevention procedure, involved contact between those who are administering the vaccine and the community,” Lovemore Makurirofa, a research and information officer at the Cancer Association of Zimbabwe, told NewsDay. “Because of the lockdown and other COVID-19 prevention mechanisms such as avoiding contact, these programmes were suspended.”
A preventable death is a tragedy that ripples outwards, tingeing the lives of the people left behind. The loss of her mother left teenaged Faith Mudangwe exposed to exploitation.
Her new custodians covertly negotiated her marriage to a potential suitor, a 70-year-old man, she says. She was not asked for her consent, and says she had never truly understood the costs of forced union, until she was officially handed over to the old man as his new bride, in exchange for a paltry bride price – some household groceries.
“I was disturbed to get married to an old man whom I respected and considered as my own grandfather,” Faith recalls. “When I arrived at my new home, I was totally confused and I really missed going to school with my friends.”
In Zimbabwe, one woman out of three is married before adulthood. Married at 14, Faith became sexually active early, which further increased her chances of sexually transmitted diseases, including –causing HPV.
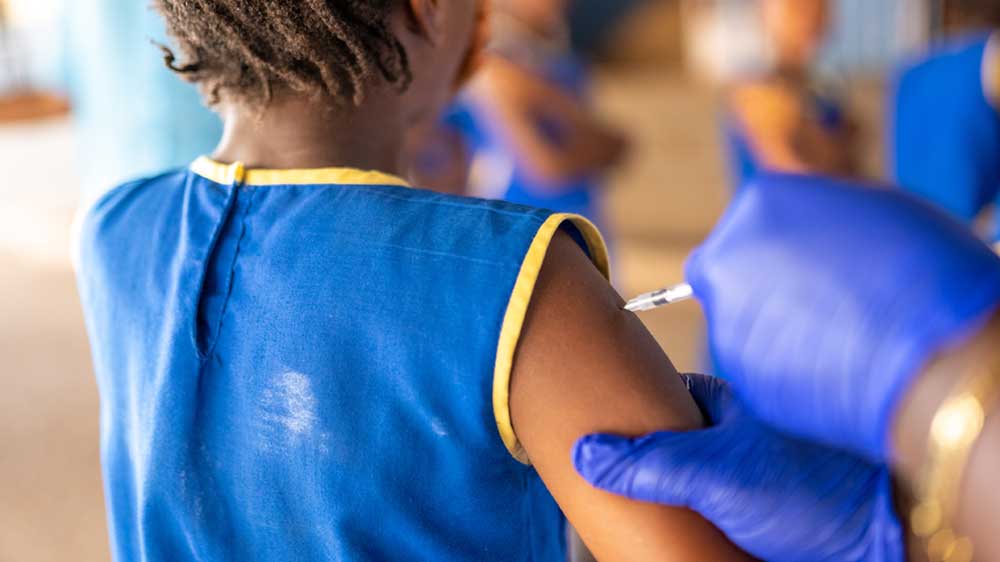
Credit: Gavi/2023/Dominique Fofanah
Vaccines sting, and they don’t protect against child marriage – but they are likely to save the lives of tens of thousands of the young generation.
Dylan Mabwe, 11, a girl from Harare, had mixed feelings about her recent tetanus and HPV vaccination jabs. “The two jabs were very painful, but I now understand it will help me have a healthy future. I watched my friends crying and running away, but we had to get vaccinated,” she said.
“We have been conducting the HPV and tetanus vaccination campaign in schools for the past few days before the schools closed down, in order to reach a wider number of students, and those who might have missed out before,” Shamiso Kitano, a health worker, said. “There was a higher turnout and reach during the campaign and most parents gave their consent. The vaccination campaign was easy for us, and we managed to reach many children.”
“The two jabs were very painful, but I now understand it will help me have a healthy future. I watched my friends crying and running away, but we had to get vaccinated.”
– Dylan Mabwe, age 11
Apart from schools, other teams focused their attention on public places like shopping malls, churches and social facilities to reach those who had missed out. At some public gatherings, the vaccination teams announced their presence for people to visit their stalls for vaccination, and other health services, like blood pressure checkups, and family planning advice.
But despite the notable success of the integrated vaccination campaign, problems persist. Even with the documented prevalence of cervical cancer in Zimbabwe, some girls from some apostolic sects still refused to get vaccinated, citing their religious beliefs. Besides that, there is a general lack of proper health information.

Credit: Elia Ntali
For Faith, now a mother of four, the scars of a stolen childhood are visible. Her speech is guarded, calculated. She says she is suspicious of strangers. She’s a survivor, however – and she means to make sure that her children get what she missed out on: “I want my children to get proper medical healthcare and get married when they are mature.”


